What Distinguishes Psoriatic Arthritis From Other Types of Arthritis?
An excellent question I often get from a lot of my patients, and even residents who rotate with me, is how I can tell the difference between psoriatic arthritis and other types of inflammatory arthritis.
Although the diagnosis can be obvious with a classic presentation in some cases, the evaluation isn’t always straightforward or simple.
The challenges of diagnosing PsA
The diagnosis can become confusing, especially with ambiguous terms such as “seronegative rheumatoid arthritis” or the possibility of having psoriatic arthritis without the typical skin manifestations.
Lab studies aren’t always helpful, either. The rheumatoid factor can be slightly elevated with psoriasis and psoriatic arthritis, which further muddles the diagnostic picture. The HLA-B27 is a genetic marker for psoriasis and psoriatic arthritis but doesn’t have a 100% correlation with the development of symptoms.
Factors to identify in diagnosing PsA
Both rheumatoid and psoriatic arthritis can cause erosions of the small joints of the hands or feet. With similarities and overlaps between psoriatic arthritis and other arthritic conditions causing joint pain and swelling, what specific clues do we have to identify the correct diagnosis?
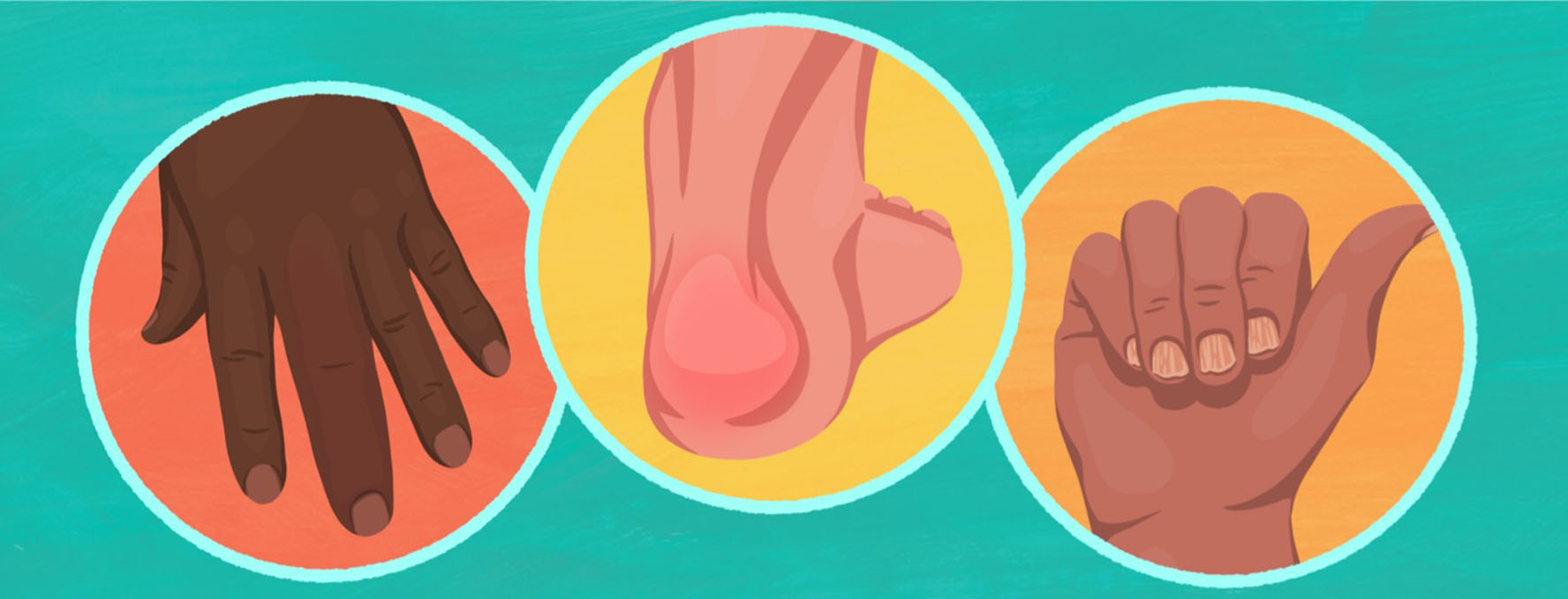
Dactylitis
The presence of dactylitis supports the diagnosis of psoriatic arthritis over rheumatoid arthritis. A feature of psoriatic arthritis that I always ask about and pay close attention to.
Also called a “sausage digit,” which is aptly named based on its appearance, dactylitis causes swelling along the entire length of a digit, such as a finger or a toe. Dactylitis is caused by swelling of a tendon and its sheath that runs along the finger or toe rather than swelling of a single joint in the hands or feet.
With the onset of dactylitis, it almost feels like a finger or toe was stubbed or injured out of the blue and starts to swell on its own, even though no injury or trigger can be identified or recalled.
Enthesitis
Enthesitis is inflammation that occurs at the insertion site of a tendon or ligament. Unique to psoriatic arthritis, enthesitis is usually found at the back of the heel at the Achilles tendon.
The rare times that I have actually gotten to see enthesitis in person, the patient had a painful lump with swelling and redness at the back of one of the heels, but not the other. Some patients have been able to capture pictures of enthesitis when it occurred and share them with me on their smartphones during appointments.
Enthesitis does not tend to occur with rheumatoid arthritis or osteoarthritis, and is considered one of the hallmark features of psoriatic arthritis.
Nail dystrophy
Nail dystrophy is the result of psoriatic arthritis, causing inflammation of the nail beds near the distal interphalangeal joints. This can have variable appearances, ranging from nail pitting leaving divots on the nail surface to wavy nails with deep ridges.
Nail dystrophy can even resemble a fungal nail infection with thick, discolored nails that break apart easily. I pay close attention to the nails of my patients with psoriatic arthritis. Rheumatoid arthritis and osteoarthritis do not cause nail changes, so the nails are a clue to the diagnosis of psoriatic arthritis.
Usually, as inflammation fades from the joints and nail beds, the nails also start to grow out more normally, which is always a great thing to witness!
This or That
Do you also find it painful to sit for extended periods of time?
Join the conversation